This post was originally published in February 2019 and was fully revised in April 2026 to reflect current trauma-informed and equity-led practices.
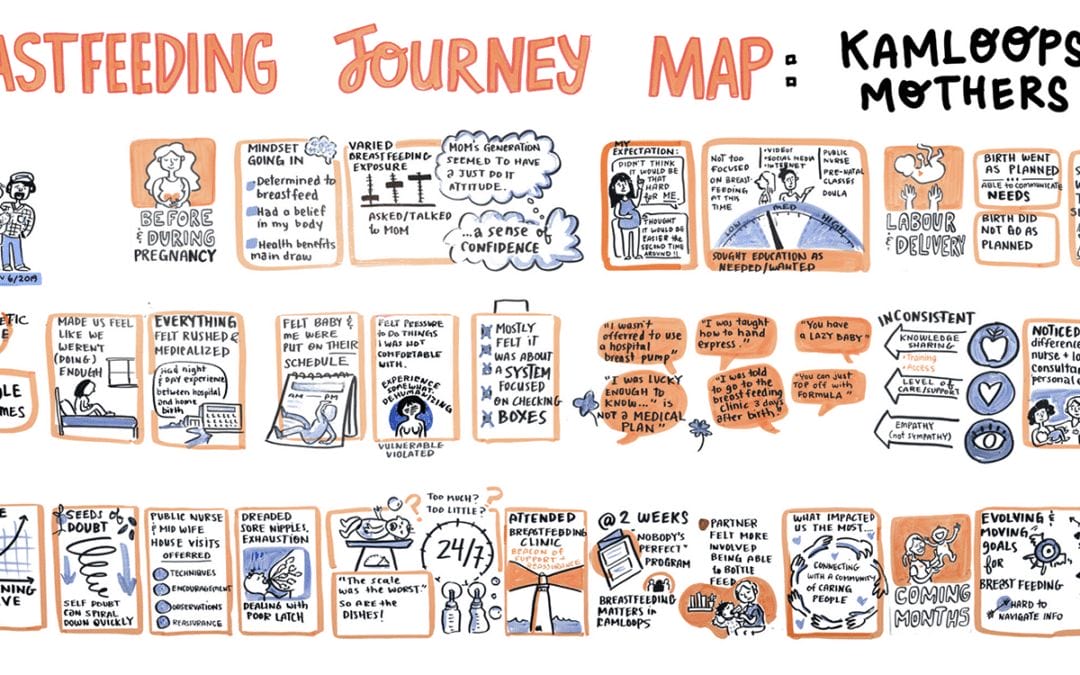
Journey mapping is a facilitated process used to understand the path(s) people follow through a service, program, or system. It is a qualitative capture, not a quantitative one; it synthesizes the voices of those with lived and living experience into a clear, accessible visual to reveal common gaps, strengths, and opportunities.
While there is no “correct” way to map, sustainable and impactful change only happens when the people receiving services are central to how we design and evaluate them. Because this process requires participants to share personal and often difficult stories, our primary responsibility is to support safety through intentional design, feedback, and relationality.
.
Supporting a Safe Space for Journey Mapping
A note on “safe spaces:” safety is a felt experience held by the participants, not a static environment we can simply build. For further learning and workshops on safe spaces, visit Cultivating Safe Spaces.
Be Transparent and Action-Oriented
Before a session begins, participants must understand the purpose and boundaries of the project. Mapping should never be a “nice-to-have” exercise; the insights gathered must be used to drive tangible system change.
→ Clarify the “Why”: Be open about how the map and its companion report will be used to advocate for funding or guide strategic planning.
→ Confidentiality: All insights will be anonymized and that their participation is entirely voluntary and will not impact their care.
→ Participation is Voluntary: Remind participants they can choose to end their involvement at any time.
Pre-Session Participant Package
Rather than just a simple invite, send a concise pre-read package or booklet. This allows participants to reflect in their own time and reduces “on-the-spot” pressure during the session. This booklet should include:
→ Prompt Questions: Thoughtful questions to help them organize their thoughts before arriving.
→ A Blank Journey Map: A template for them to jot down milestones or feelings.
→ Self-Care Guidance: Acknowledge that reflecting on these journeys can be difficult and provide tips for emotional grounding.
→ Facilitation Team Intro: A short video or bio of the facilitation team helps put a face to the names and builds early rapport.

“What Helps You Feel Supported?”
Safety is not a “one-size-fits-all” concept. Avoid assumptions and remain curious and flexible about what participants need.
→ Ask Directly: Seek input on what helps people feel supported, whether it’s frequent breaks, neutral locations, or specific accessibility supports.
→ Community Partnership: When working with specific communities, collaborate with a community member or co-facilitator to design the tone and format.
Indigenous Gatherings and Relationality
If gathering insights from Indigenous participants, the process must be relational and co-designed.
→ Respect OCAP® Principles: Understand that First Nations people have Ownership, Control, Access, and Possession over their data, and that the journey mapping project must be grounded in these principles.
→ Lead with Indigenous Voice: Sessions should be led or co-led by Indigenous facilitators or Designers, and with an Elder present to open and close the session in a good way .

The Meeting Space
The physical or virtual environment influences the process tremendously.
→ Neutral, Quiet Space: Avoid clinical settings that may be triggering for those who have experienced medical trauma. Choose a space that is quiet and has natural light.
→ Comfort and Movement: Use a u-shape of chairs so everyone can see the map and each other. Encourage movement by providing alternative seating like cushions or beanbag chairs.
→ Sensory Supports: Provide “fidget items” (pipe cleaners, stress balls) and paper for doodling to aid deep thinking. Doodling is proven to aid in thinking, so pens and paper are great additions.
→ Accessibility: Is the space accessible? On a bus route or with parking available? Are you asking participants to travel great distances?
No Observers
To maintain an equitable and safe space, journey mapping is not a forum for observers. Everyone in the room must be a participant, a chosen support person, or part of the facilitation team. Be mindful of power imbalances; people are less likely to share openly if management or leadership is present.

Co-Creating Shared Values
Begin every session by co-developing a set of shared values (e.g., listening with care, respecting unique perspectives, and maintaining confidentiality). These should be captured visually by the graphic facilitator for everyone to see.
Intentional Facilitation & Mapping Style
Using a Graphic Facilitator helps participants feel seen and heard in real time.
→ Visual Synthesis: The graphic facilitator organizes complex stories into a clear summary using layout, colour, and visuals authentic to the experiences shared.
Visual maps are highly effective at facilitating understanding of complex journeys, picking out milestones at-a-glance, and also conveying the emotion of the journey. Participants will more readily connect to the map, can easily identify areas where more detail is needed.

Supporting Quieter Voices
→ Anonymous Input: Provide sticky notes for those who prefer to write down thoughts rather than speak them in the group.
→ Participant Booklets: Provide notebooks or prompt questions that participants can use to share insights privately.

Compensation and Reciprocity
Recognize the value of people’s time and lived experience.
→ Fair Pay: Participants, Elders, and community partners should be compensated for their time and contributions. This should be payment, or cash gift-cards. This guide from BC Cancer is a helpful starting place.
→ The Validation Loop: Within one week, provide participants with a draft digital image of the map to confirm accuracy and suggest final changes .

Facilitator Self-Care
Supporting others through traumatic stories takes immense energy. Ensure the facilitation team has a plan for debriefing after the session to discuss emerging themes and emotional impacts.